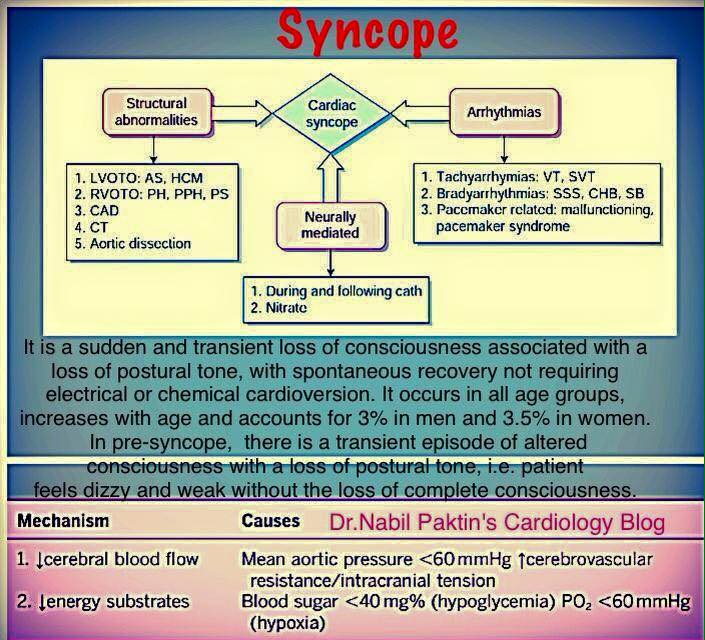
In itself, ‘syncope’ is not a complete diagnosis. These are often termed ‘syncope mimics’ or ‘pseudosyncope’, but differ from syncope inasmuch as they do not cause true loss of consciousness (e.g., conversion reactions, malingering, and cataplexy). Each of these differ from syncope either by the need for medical intervention to reverse the process (e.g., hypoglycemia) or by the underlying mechanism of the loss of consciousness (e.g., electrical disturbance in epilepsy, trauma in head injury, etc.) or both. In this regard, it is important to note that other conditions (e.g., epilepsy, concussions, metabolic disturbances and intoxications) may also cause a temporary loss of consciousness (T-LOC) but nonetheless are not ‘syncope’ ( 3- 5). 
Minneapolis, MN, 55455Įmail is a syndrome in which a relatively sudden-onset, brief loss of consciousness results from a temporary self-terminating period of total cerebral hypoperfusion ( 1- 4). 
From the Cardiac Arrhythmia Center, Cardiovascular Division, Department of Medicine, University of Minnesota Medical School, MMC 508, 420 Delaware Street SE, Minneapolis, MN 55455, USA.Ĭorrespondence: David G Benditt MD. Professor of Medicine, Co-Director Cardiac Arrhythmia Center, University of Minnesota Medical School. 2012 47(5):362-365.Syncope: an overview of diagnosis and treatmentĭavid G Benditt. Cases of pediatric narcolepsy after misdiagnoses. Narcolepsy: signs, symptoms, differential diagnosis, and management. Complex movement disorders at disease onset in childhood narcolepsy with cataplexy. Impact of obesity in children with narcolepsy. Inocente CO, Lavault S, Lecendreux M, et al.Reducing the clinical and socioeconomic burden of narcolepsy by earlier diagnosis and effective treatment. Cataplexy features in childhood narcolepsy. Serra L, Montagna P, Mignot E, Lugaresi E, Plazzi G.Sleep in children with attention-deficit/hyperactivity disorder: meta-analysis of subjective and objective studies. Cortese S, Faraone SV, Konofal E, Lecendreux M.Darien, IL: American Academy of Sleep Medicine 2014. In: The International Classification of Sleep Disorders – Third Edition (ICSD-3) Online Version. Listening to the patient voice in narcolepsy: diagnostic delay, disease burden, and treatment efficacy. Maski K, Steinhart E, Williams D, et al.The clinical spectrum of childhood narcolepsy. Postiglione E, Antelmi E, Pizza F, Lecendreux M, Dauvilliers Y, Plazzi G.Clinical and therapeutic aspects of childhood narcolepsy-cataplexy: a retrospective study of 51 children. Aran A, Einen M, Lin L, Plazzi G, Nishino S, Mignot E.Cataplexy and its mimics: clinical recognition and management. Pillen S, Pizza F, Dhondt K, Scammell TE, Overeem S.Patients’ journeys to a narcolepsy diagnosis: a physician survey and retrospective chart review. 
Narcolepsy in children: a diagnostic and management approach. Insomnia, parasomnias, and narcolepsy in children: clinical features, diagnosis, and management. Narcolepsy with cataplexy is often confused with Sydenham chorea or PANDAS due to overlap of certain characteristics, such as episodic course, childhood onset with acute presentation following streptococcal infection, and coexistence of motor and behavioral symptoms that present similarly to cataplexy in narcolepsy in pediatric patients.Sydenham chorea and pediatric autoimmune neuropsychiatric disorder associated with streptococcal infections (PANDAS) are brain autoimmune poststreptococcal diseases that occur in pediatric patients.Preserved consciousness distinguishes cataplexy from syncope.To differentiate cataplexy attacks from syncope, thorough screening for cardiac arrhythmias, head up tilt table testing, and video recordings of the attacks may be necessary.Loss of muscle tone and rapid recovery associated with cataplexy may be confused with syncope.Close to disease onset, cataplexy can mimic a spectrum of motor disorders and muscle diseases resulting in a misdiagnosis of myopathy.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
